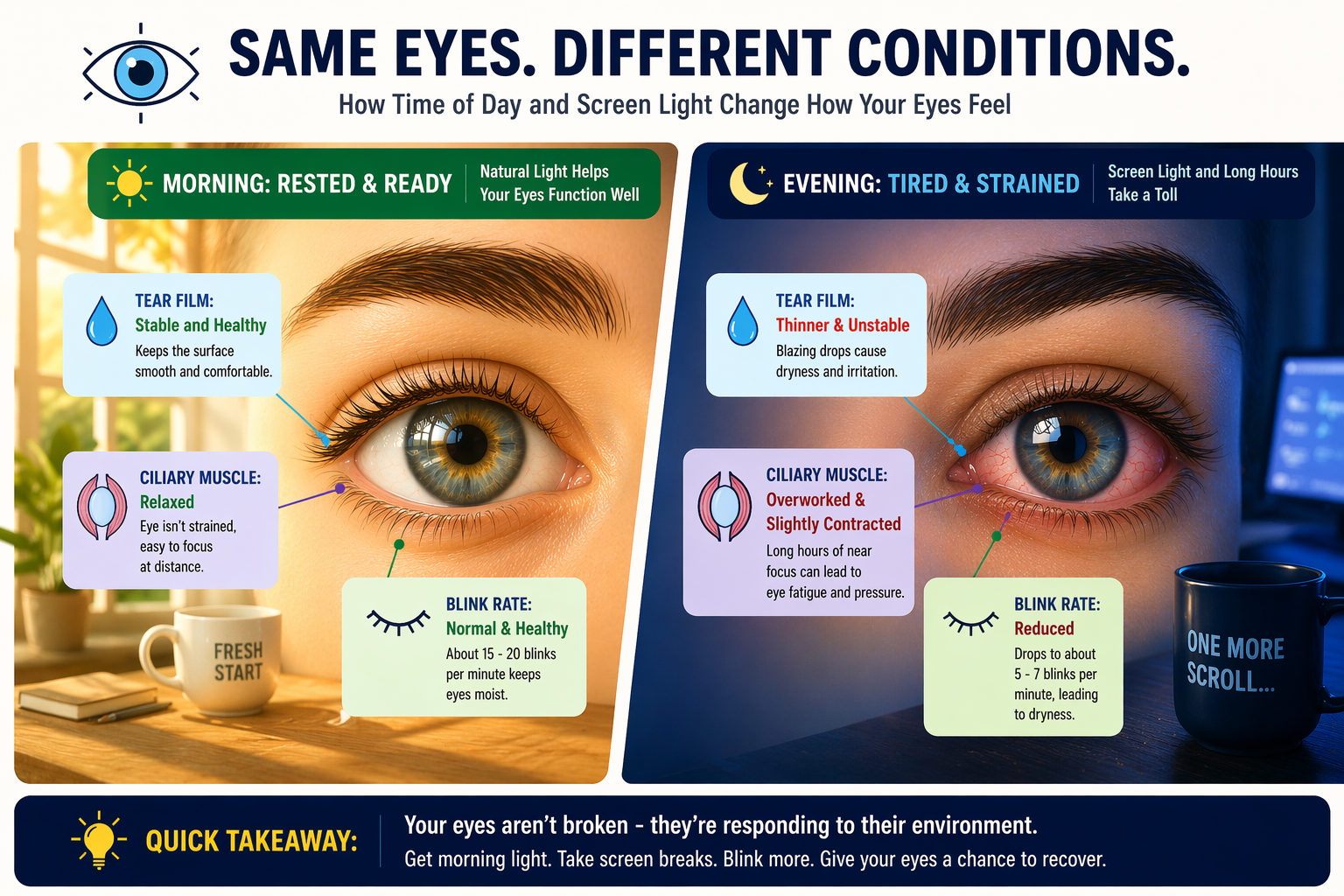
Eyes that feel comfortable in the morning but deteriorate by evening are responding to a combination of accumulated visual fatigue, reduced blink rate from screen use, shifting cortisol levels, and lacrimal gland depletion throughout the day. This pattern is extremely common and often reflects underlying dry eye syndrome, binocular vision dysfunction, or uncompensated refractive error rather than random discomfort.
You wake up, your eyes feel clear. By 9 PM, they’re burning, blurry, or heavy. If this cycle repeats itself daily, it’s not a coincidence. Your visual system is telling you something specific about how it’s being used and what it needs. Understanding that pattern is the first step toward actually fixing it.
Key Takeaways
- Morning eye comfort is largely due to overnight tear replenishment and rest for the ciliary muscles responsible for focusing.
- Evening eye strain accumulates from hours of screen use, reduced blinking, and the progressive depletion of the tear film.
- Cortisol follows a natural daily rhythm that affects ocular surface inflammation, often making symptoms noticeably worse after mid-afternoon.
- Undiagnosed binocular vision issues or uncorrected prescriptions are frequently the hidden driver behind worsening evening vision symptoms.
- Simple habit adjustments combined with a professional eye assessment can dramatically reduce or eliminate the morning-to-night symptom gap.
- Persistent evening symptoms that don’t improve with rest or hydration should be evaluated by a vision specialist, not managed with over-the-counter drops alone.
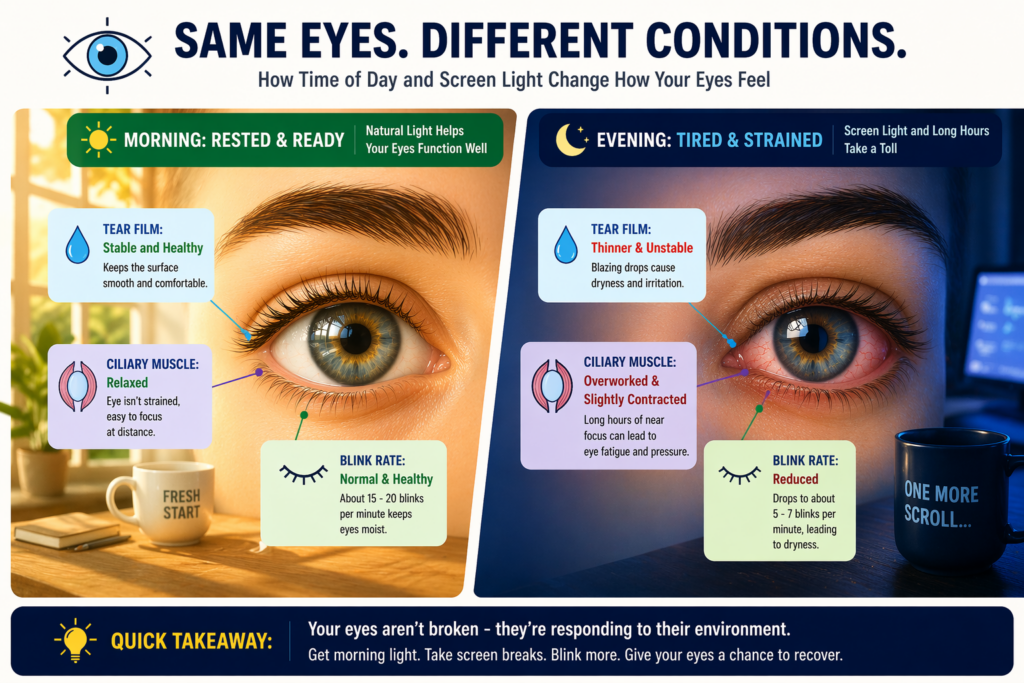
What Actually Happens to Your Eyes While You Sleep?
During sleep, your eyes are closed, protected, and largely stationary. The lacrimal glands refill your tear reservoir, the ciliary muscles that control lens shape fully relax, and any mild surface inflammation from the previous day gets a chance to calm down. You wake up with what is essentially a reset visual system.
That reset is temporary. The moment you begin demanding focused visual work, the depletion process starts again. Most people don’t notice it for several hours because the reserves are full and the muscles are fresh. The degradation happens gradually and doesn’t become symptomatic until a threshold is crossed, which for most people lands somewhere in the late afternoon or evening.
Why Does Visual Fatigue Build Up Throughout the Day?
Research consistently shows that the average office worker blinks approximately 15 to 20 times per minute at rest, but that rate drops to as low as 5 to 7 times per minute during focused screen use. Each blink spreads a fresh layer of the tear film across the corneal surface. Fewer blinks mean the tear film evaporates faster, and the corneal surface becomes irregular, which scatters light and causes blurred vision and burning sensations.
The ciliary muscle, a small ring of muscle inside the eye responsible for adjusting lens curvature, is constantly contracting when you focus on close distances. After hours of computer work, reading, or phone use, this muscle becomes fatigued in a way that is directly analogous to how your calf feels after a long run. The technical term for this is accommodative fatigue, and it explains why text looks blurry or swimmy by the end of a workday even if your prescription is correct.
Studies on digital eye strain estimate that more than 65% of people who use screens for more than 4 hours daily experience symptoms including eye fatigue, dryness, headaches, and blurred vision, with symptoms peaking in the late afternoon and early evening hours.
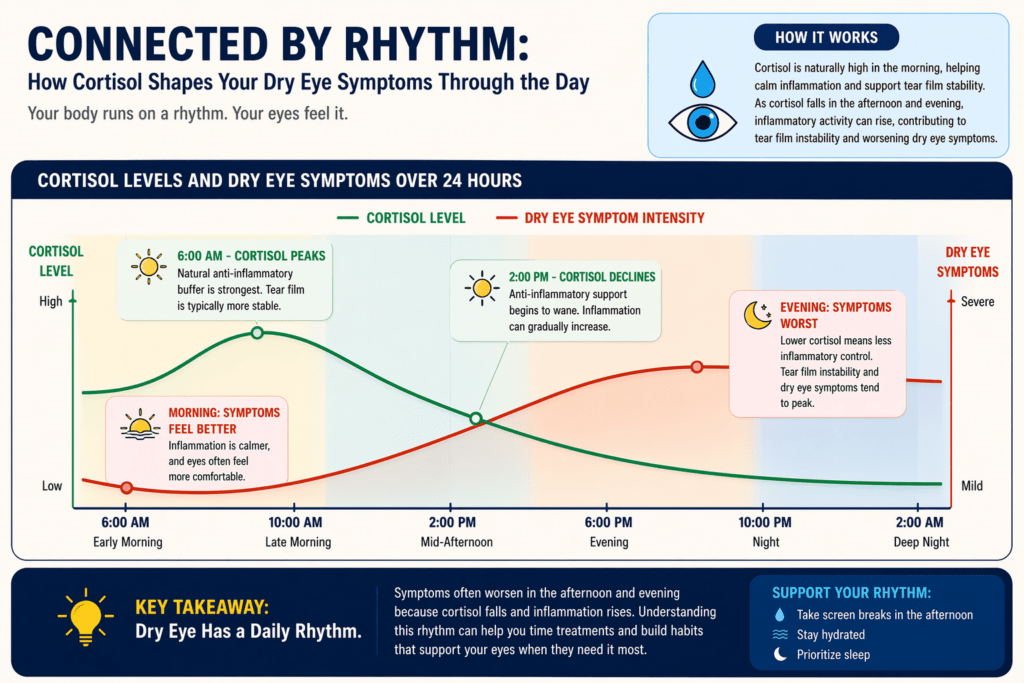
The Role of Cortisol in Your Eye Comfort
Cortisol follows a predictable daily arc. It peaks sharply in the early morning hours, which is one reason why many inflammatory conditions feel more manageable in the first half of the day. By mid-afternoon, cortisol drops, and with it, some of the natural anti-inflammatory buffering it provides.
Ocular surface inflammation, a core feature of chronic dry eye disease, is modulated in part by systemic cortisol levels. The meibomian glands, which produce the oily outer layer of the tear film, are sensitive to inflammatory signaling. As daytime cortisol falls and inflammation becomes less suppressed, tear film instability tends to increase, which is one physiological reason why dry eye symptoms characteristically worsen toward evening.
This doesn’t mean high cortisol is always good for your eyes. Chronically elevated cortisol from prolonged stress can actually damage meibomian gland function over time and raise intraocular pressure. The relationship is about the natural daily rhythm of cortisol, not the absolute level.
Common Reasons Your Eyes Feel Worse at Night
| Cause | What’s Happening | When It Peaks |
| Tear film depletion | Reduced blinking during screens evaporates tears faster than they’re replenished | Late afternoon onward |
| Accommodative fatigue | Ciliary muscles exhausted from hours of close-focus work | After 4+ hours of screen use |
| Cortisol drop | Natural anti-inflammatory buffer weakens; ocular surface inflammation increases | Mid-afternoon to evening |
| Binocular vision strain | Eye teaming effort accumulates when convergence or tracking muscles are struggling | End of workday or school day |
| Blue light and glare | Evening screen sessions in darker rooms increase pupil dilation and contrast strain | Night screen use |
| Contact lens wear | Lenses absorb tear film moisture throughout the day, drying out by evening | After 8+ hours of wear |
How Binocular Vision Problems Amplify Evening Symptoms
One of the most underdiagnosed contributors to progressive evening eye fatigue is a problem with eye teaming. When your two eyes don’t point at exactly the same target naturally, the visual system has to apply constant corrective muscle effort to fuse the two images into one. This compensation is largely invisible because people adapt to it, but it demands ongoing neurological and muscular work.
In the morning, after rest, that compensatory effort is manageable. By evening, after a full day of sustained effort, the system starts to break down. This often shows up as double vision, words that seem to move on the page, headaches centered around the temples or behind the eyes, or the feeling that focusing requires actual effort. If this pattern sounds familiar, a functional vision assessment rather than a standard eye chart test is what you need.
Step-by-Step: How to Reduce Evening Eye Fatigue
- Apply the 20-20-20 rule consistently. Every 20 minutes of screen use, look at something 20 feet away for 20 seconds. This relaxes the ciliary muscle and gives it a brief but meaningful recovery window.
- Audit your blinking habits. Set a reminder every 30 minutes to consciously perform several complete, deliberate blinks. Partial blinks are common during screen use and don’t effectively spread the tear film.
- Reduce screen brightness after 6 PM. A screen that’s significantly brighter than your surrounding environment forces the iris to work harder to manage contrast, adding to end-of-day fatigue.
- Use preservative-free lubricating drops midday. Don’t wait until your eyes are burning to use drops. A midday application around the 4-5 hour mark of screen use can reset the tear film before depletion becomes symptomatic.
- Check your screen distance and monitor height. Eyes held in a slightly downward gaze expose less corneal surface and reduce evaporation. Screens positioned at or slightly below eye level also reduce the sustained upward gaze that increases surface exposure.
- Book a functional vision assessment. If lifestyle adjustments don’t fully resolve the morning-to-night symptom gap within two to three weeks, the issue may be structural rather than habitual. Problems with visual alignment or meibomian gland function require professional evaluation to address properly.
What Are Common Mistakes People Make When Managing This?
- Relying solely on over-the-counter redness relief drops. Drops containing vasoconstrictors reduce redness cosmetically but do nothing for the underlying tear film issue and can cause rebound redness with regular use.
- Assuming the problem is purely the screen. Screens accelerate tear evaporation and accommodative fatigue, but they don’t create the underlying vulnerability. An uncompensated prescription, meibomian gland dysfunction, or binocular vision problem is usually what makes someone symptomatic while others using the same screens are not.
- Treating dry eye with hydration alone. Drinking more water helps systemic hydration but does not meaningfully change tear film composition. The oily lipid layer, which prevents evaporation, comes from meibomian glands, not from systemic fluid intake.
- Ignoring the posture and neck connection. Chronic neck tension and forward head posture restrict blood flow and alter the neurological signals reaching the visual system, contributing to eye fatigue in ways that eye drops will never address.
- Waiting years before seeking an assessment. Many people normalize progressive evening eye discomfort as “just part of aging” or “just screens” for years before discovering an underlying condition that was highly treatable.

Diet, Inflammation, and Your Evening Eye Symptoms
Diets high in refined sugars and omega-6 fatty acids have been associated with increased systemic inflammation, which can worsen meibomian gland dysfunction and dry eye severity. Omega-3 fatty acids, particularly EPA and DHA found in fatty fish and high-quality supplements, have shown statistically significant improvements in tear film stability and dry eye symptom scores in randomized controlled trials.
This doesn’t mean diet is the primary driver of your evening symptoms, but it does mean that persistent inflammation from poor dietary patterns can lower your threshold for discomfort. People who already have borderline tear film stability become symptomatic earlier and more intensely when systemic inflammation is elevated.
When Should You Be Concerned Rather Than Just Inconvenienced?
Gradual, predictable worsening across the day is almost always benign and addressable. There are, however, symptoms that warrant prompt evaluation rather than lifestyle management.
| Symptom Pattern | Likely Explanation | Urgency |
| Burning and dryness worsening by evening | Dry eye syndrome, meibomian gland dysfunction | Schedule within a few weeks |
| Blurry vision that clears with blinking | Tear film instability, mucin layer deficiency | Schedule within a few weeks |
| Double vision or words shifting on the page | Binocular vision dysfunction | Prioritize assessment soon |
| Sudden vision change or loss in one eye | Vascular event, neurological cause | Emergency evaluation immediately |
| Visual disturbances with limb weakness or speech difficulty | Potential neurological emergency | Emergency evaluation immediately |
Frequently Asked Questions
Why do my eyes feel worse at night?
By evening, your tear film has been depleted through hours of reduced blinking, your ciliary muscles are fatigued from sustained near focus, and your cortisol levels have dropped, removing some of the anti-inflammatory buffering that kept symptoms manageable earlier in the day. If you also have a mild binocular vision issue or a prescription that’s slightly off, those problems become impossible to compensate for once fatigue accumulates. The morning reset from sleep temporarily hides the underlying vulnerability.
What are the first signs of MS in the eyes?
Optic neuritis, an inflammation of the optic nerve, is often among the earliest neurological symptoms of multiple sclerosis. It typically presents as pain behind one eye that worsens with eye movement, followed by a reduction in central vision or color desaturation, particularly a dimming of red tones. Symptoms usually affect one eye at a time rather than both simultaneously. Anyone experiencing sudden unilateral vision changes with eye movement pain should seek prompt neurological evaluation, as this is distinct from ordinary eye fatigue.
What is the #1 worst food for vision loss?
Ultra-processed foods high in refined sugars and trans fats are consistently associated with the highest risk of accelerated vision deterioration in research literature. The combination of chronic blood sugar spikes and systemic inflammation directly damages the microvascular structures supplying the retina, which is why diabetic retinopathy is one of the leading causes of preventable vision loss globally. Heavily sweetened beverages and packaged snacks with partially hydrogenated oils are particularly problematic for long-term retinal health. You can also explore how presbyopia eye drops and age-related changes interact with overall visual health as part of a broader prevention conversation.
Can cortisol affect your eyes?
Yes, in several meaningful ways. Acutely elevated cortisol from stress can temporarily raise intraocular pressure, which is relevant for people with glaucoma or glaucoma risk. Chronically elevated cortisol impairs meibomian gland function and can worsen tear film instability over time. The natural daily drop in cortisol after mid-afternoon also removes some anti-inflammatory support from the ocular surface, which is one reason dry eye symptoms tend to peak in the evening rather than the morning.
What are 10 warning signs of high cortisol?
Persistent high cortisol, often called hypercortisolism or Cushing’s syndrome in clinical contexts, can present with weight gain concentrated around the abdomen and face, high blood pressure, muscle weakness particularly in the thighs and shoulders, mood changes including anxiety and depression, poor sleep despite fatigue, slow wound healing, easy bruising, increased thirst and urination, headaches, and blurred or fluctuating vision. If you’re experiencing several of these together and your eye symptoms don’t follow a simple fatigue pattern, it’s worth discussing systemic cortisol assessment with a physician alongside your eye evaluation.
What This All Means for Your Eyes Tonight
The morning-to-night pattern your eyes follow isn’t random discomfort. It’s a repeatable, physiologically logical response to how your visual system is being used and what’s limiting its ability to recover throughout the day. Identifying whether the dominant driver is tear film depletion, accommodative fatigue, a binocular vision issue, or systemic inflammation makes the path forward much clearer than treating all evening eye symptoms the same way.
Lifestyle adjustments help. Proper blinking habits, strategic lubricating drops, screen ergonomics, and reducing dietary inflammation all move the needle. But when the gap between your morning and evening eye comfort is significant and persistent, the most reliable next step is a thorough functional vision assessment that goes beyond checking the letters on a chart.
At Opto-Mization, the team specializes in identifying the functional and structural causes behind patterns exactly like this one. Whether it’s dry eye management, a binocular vision assessment, or a prescription evaluation that accounts for how your eyes perform after a full workday rather than just at 9 AM, the goal is to get your evening comfort matching your morning baseline. Call +1 778-608-5982 to book your assessment and stop normalizing something that doesn’t have to feel that way.